-
Contact lenses (CLs) are among the most widely used biomedical devices globally, employed for both vision correction and cosmetic purposes1. These transparent, hemispherical lenses are worn directly on the cornea, offering a broader field of view and improved quality of life compared to traditional spectacles2. The conceptual foundation of CLs can be traced back to 1508, when Leonardo da Vinci proposed altering corneal power by viewing through a water-filled glass bowl an idea that inspired subsequent innovations in optical correction3.
The contact lens industry has since grown into a substantial sector of the medical device market, valued at approximately $12.8 billion in 2019, with an expected compound annual growth rate (CAGR) of 5% from 2020 to 20274, 5. This growth is driven by increasing demand for comfort, aesthetics, and improved visual performance. Early lenses were fabricated using rigid materials, but advances in polymer science have led to the widespread adoption of soft lenses made from hydrogels, silicone hydrogels, and hybrid composites6. Material selection is guided by user requirements such as oxygen permeability, water content, wettability, mechanical durability, and biocompatibility7. Among these, hydrogels are particularly valued for their softness, hydration capacity, and oxygen transmissibility, closely mimicking ocular tissue. Hydrogels have further gained prominence for their biocompatibility, high water content, and mechanical flexibility, enhancing wearer comfort and functionality8. Moreover, hydrogel-based lenses are being engineered with multifunctional capabilities, including extended wear, real-time health monitoring, and ocular drug delivery9, 10. However, conventional hydrogel lenses often suffer from limited mechanical strength, suboptimal moisture retention, and discomfort during extended use.
To address these limitations, next-generation materials such as silicone hydrogels, hydrogel composites have been explored, offering improvements in oxygen transmission, hydration, and structural resilience11–20. These material innovations continue to shape the development of advanced CLs that meet evolving clinical and user requirements. Recent studies have explored the fabrication of hydrogel-based contact lenses for diverse ocular applications. Alam et al.20 developed 3D-printed hydrogel lenses using in situ synthesized pHEMA doped with wavelength-selective dyes (Atto 565 and 488) to correct color vision deficiency (CVD), filtering 80%-90% of targeted wavelengths and enhancing color perception as validated by the Ishihara test. Similarly, Elsherif et al.11 fabricated soft hydrogel lenses that blocked over 95% of undesired wavelengths, demonstrating long-term dye stability. Salih et al.12, 13 introduced gold and silver nanoparticle embedded pHEMA lenses for red-green and blue-yellow CVD, respectively, showing performance comparable to commercial filters and improved water retention and wettability. Further advancements include customized 3D-printed intraocular lenses by Alam et al.14, which demonstrated ~50% wavelength filtering at 565 nm with high optical transparency and polarization-independent transmission. Hisham et al.15 developed 4D-printed photochromic hydrogel lenses responsive to UV light for dynamic optical modulation, offering UV protection and hazard alerting. Additionally, Hisham et al.16 developed a low-cost vat photopolymerization method for multi-material customization on commercial lenses. Salih et al. engineered smart contact lenses with integrated chromogenic materials into pHEMA, enabling UV and temperature-responsive behavior, with tunable light blocking and colorimetric transitions17. Furthermore, Hisham et al.18 demonstrated multiband optical filtration using Atto dyes in hydrogel-based multimaterial 3D-printed lenses. Sakr et al.19 developed multifunctional lenses combining color filtering and pH sensing via a novel multimaterial 3D printing approach. Collectively, these works highlight the versatility of hydrogels for noninvasive therapeutic and diagnostic ocular applications.
Traditionally, CLs have been manufactured using lathe cutting, spin casting, and cast molding6. While effective, these methods are often application-specific, labor-intensive, and require post-processing. Additive manufacturing, particularly 3D printing, has emerged as a powerful alternative, offering greater design flexibility and rapid customization. Digital Light Processing (DLP) stands out among 3D printing technologies for its high-resolution, layer-by-layer fabrication, and ability to produce complex geometries. DLP enables precise control over UV exposure, supports multimaterial printing, and is compatible with custom resin formulations, making it especially suitable for ophthalmic applications21, 22. The technique allows for the simultaneous fabrication of multiple lenses with high spatial fidelity, enabling the scalable production of patient-specific designs. Its utility has been demonstrated in fabricating leakage-free tinted lenses with excellent optical and physicochemical stability20, establishing DLP as a preferred technique in contemporary ocular wearables.
Despite the numerous advantages of 3D printing for contact lens (CL) fabrication, the literature highlights specific limitations, particularly related to surface quality and structural integrity23, 24. A major issue arises from the stair-stepping (or staircase) effect, which is an artifact of the layer-by-layer printing process for contact lenses. This occurs not due to errors in the fabrication mechanism itself but because of the slicing strategy applied to the CAD model. When a 3D model is Fed into discrete layers for fabrication, each slice undergoes individual polymerization. Consequently, successive layers are deposited atop the previously cured ones, often creating visible step-like edges and weak interlayer bonds25, 26. These weak attachment points, especially prevalent in curved geometries, can compromise the optical clarity and mechanical durability of the lens, rendering it susceptible to failure during handling or wear. Such concerns have been reported in previous studies by Alam et al., Hisham et al., and others15, 18, 25–27.
Additionally, slicing artifacts can lead to geometrical inaccuracies, known as containment errors. Since layer thickness is typically uniform throughout the build, it does not always conform precisely to the geometry of curved surfaces. This mismatch causes the printed slices to deviate either from falling inside or outside the intended contour, thus compromising the accuracy and fit of the final structure28. The cumulative effect of these issues is a rough surface finish, which is particularly undesirable in CLs. Surface roughness not only scatters incident light, reducing visual clarity, but also negatively impacts wearer comfort29. Importantly, lens transparency is inversely related to surface roughness; smoother surfaces yield higher optical clarity, an essential requirement for functional contact lenses. This gap in current manufacturing capabilities motivates the present study, which aims to explore alternative strategies to mitigate such defects.
Several strategies have been proposed to mitigate the staircase effect30, such as reducing layer thickness, modifying print orientation (e.g., tilting relative to the z-axis), and applying post-processing treatments like solvent etching (e.g., with acetone) or resin overcoating followed by UV curing, as proposed by Formlabs6, 25, 29. These approaches collectively offer promising pathways to enhance surface smoothness, improve interlayer bonding and optical performance of 3D-printed CLs.
Despite recent advancements, achieving an optimal balance of mechanical strength, transparency, wettability, and biostability remains a considerable challenge. Furthermore, current approaches often rely on post-processing rather than integrated design strategies. To address this gap, the present study introduces a novel conformal ocular disc architecture inspired by auxetic and mechanical metamaterial principles, fabricated via DLP-based 3D printing using an in-house hydrogel formulation. While it’s not claimed that the disc exhibits a true auxetic response (e.g., a bulk negative Poisson’s ratio), its deformation mechanism intentionally draws from these architectures, incorporating rotational ligament units that enable curvature-adaptive compliance (reader is referred to section S1, Supplementary Material). This design allows precise control over disc geometry, promoting enhanced mechanical resilience, optical clarity, and enabling the flat disc to conform seamlessly to the corneal surface without requiring pre-curvature or complex post-processing. A key innovation of this work is the incorporation of a circumferential auxetic-inspired ligament network into the lens architecture. This design enables a perfectly flat-printed, conformal auxetic inspired metamaterial ocular disc into a structure that can stretch and conform seamlessly to the curved ocular surface, thereby enhancing adaptability and wearer comfort. Precise control over geometry and microstructure allows for optimization of mechanical, optical, and surface properties within a single fabrication workflow. The printed novel ocular discs are subjected to extensive characterization. Mechanical robustness was evaluated via uniaxial tensile, compressive, flexural, and tear testing. Optical performance was assessed using UV-vis transmittance and absorbance spectroscopy. Surface morphology and hydration behavior were characterized through laser profilometry, static contact angle, and swelling kinetics. In addition, material composition and stability were analyzed using Fourier-transform infrared spectroscopy (FTIR), differential scanning calorimetry (DSC), thermogravimetric analysis (TGA), and rheology. The proposed 3D printable flat lens geometry facilitates conformal contact lens printing, with minimal ocular surface coverage while delivering suitable optical performance.
By integrating design driven innovation with comprehensive multi-domain characterization, this work presents a robust platform for the development of next-generation, patient-specific contact lenses via 3D printing. The findings are anticipated to guide future advancements in material selection, structural optimization, and additive manufacturing strategies for high-performance ophthalmic devices.
-
The in-house formulated resin for 3D printing of conformal auxetic-inspired metamaterial hydrogel ocular disc was prepared using 2-hydroxyethyl methacrylate (HEMA) as the monomer, poly (ethylene glycol) diacrylate (PEGDA) as the crosslinker, and trimethyl benzoyl diphenyl phosphine oxide (TPO) as the photoinitiator (Allplace Co., Ltd., Shandong, China). All chemicals were used as received without further purification. Phosphate-buffered saline (PBS) solutions used for hydration studies were prepared by dissolving PBS tablets (Sigma-Aldrich) in deionized (DI) water according to the manufacturer’s protocol. For visualization, alcohol-based inks in magenta (B031) and parakeet green (B041) were sourced from a commercial supplier (Piccaso, UAE). Additional materials included ethanol, deionized water, and a smooth, transparent poly vinyl chloride (PVC) film.
To enable customized hydrogel fabrication via digital light processing (DLP) 3D printing, a photocurable resin was formulated and optimized for suitability with the desktop 3D printer. The resin was prepared by mixing HEMA and PEGDA in a 97:3 weight ratio, along with 1 wt.% of TPO as the photoinitiator to initiate the photopolymerization reaction. These components were stirred in a beaker at ambient conditions (~26 °C) for 15 minutes using a magnetic stirrer to ensure homogeneity as shown in Fig. 1a. To prevent premature polymerization, the beaker was shielded from ambient light using aluminum foil. The prepared resin was subsequently used for direct 3D printing of conformal auxetic-inspired metamaterial hydrogel ocular discs.
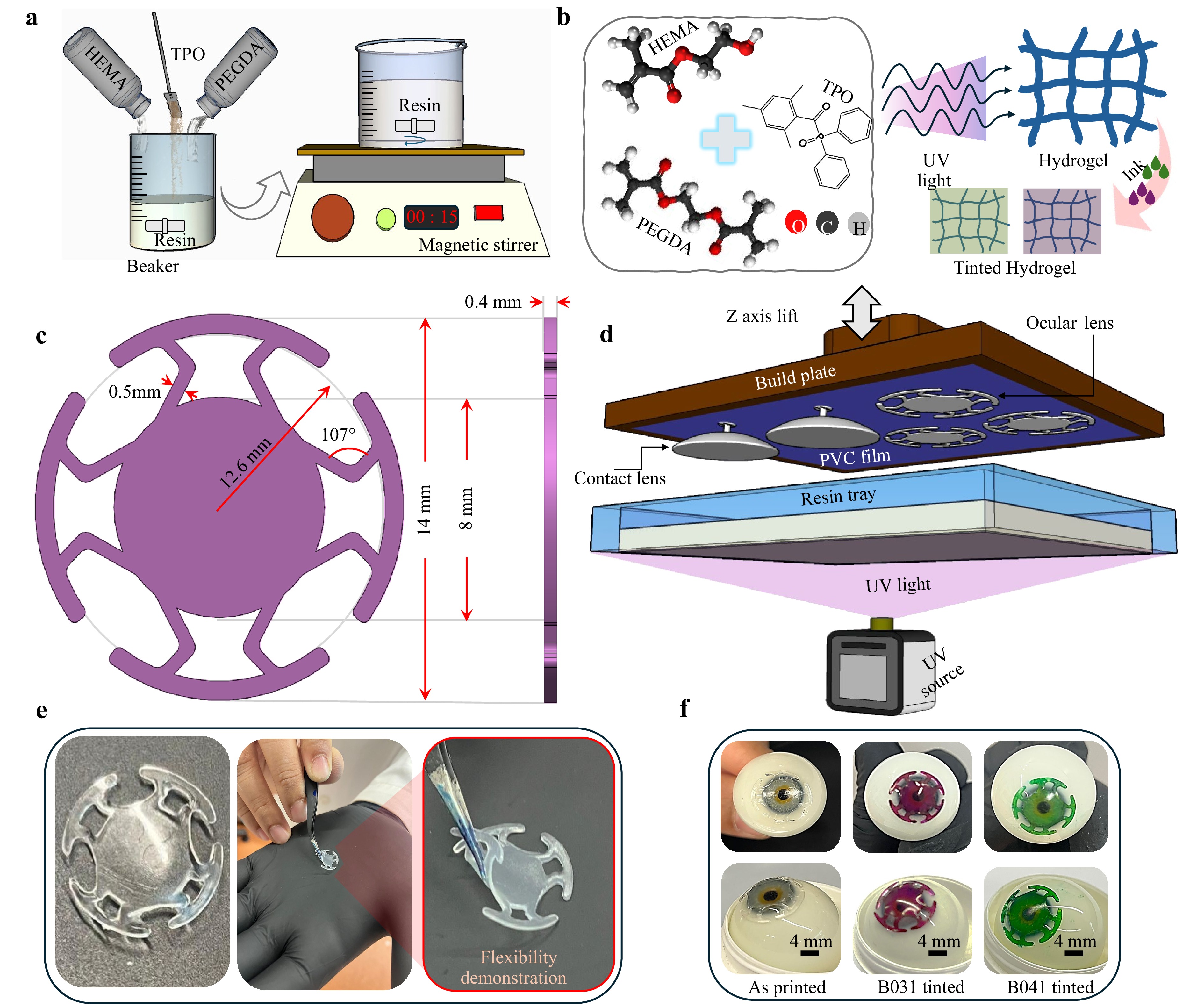
Fig. 1 Schematic overview of the fabrication process and design of the 3D printed ocular disc: a in-house preparation of the photocurable resin, b formulation of the hydrogel-based resin blend, c design specifications of the novel ocular disc geometry with an auxetic-inspired ligament network, d digital light processing (DLP) 3D printing of contact lenses and ocular discs, e demonstration of flexibility of the conformal 3D printed ocular disc, and f tinted 3D printed ocular disc using piccassio ink for ocular applications.
-
This study introduces a novel conformal auxetic-inspired metamaterial hydrogel ocular disc, designed and inspired by metamaterial principles, incorporating circumferential auxetic ligaments to enhance conformability to the eye’s hemispherical surface (Fig. 1c). The design is characterized by an overall diameter (D) of 14 mm, a wall thickness (t) of 400 µm, and additional architectural features defined by ligament thickness $ {t}_{l} $ of 500 µm and interior angle $ {\theta }_{l} $ of 107° (see Fig. 1c).
Metamaterials are broadly defined as structures whose functional response is governed primarily by geometry rather than material composition31, 32. The design philosophy of the present ocular disc aligns directly with this paradigm. As illustrated in Fig. 1f and Video S1, the disc’s ability to conform onto a hemispherical corneal surface does not originate from the hydrogel polymer alone; instead, it is the architected geometry, specifically the radial ligaments and circumferential ring, that provides the necessary degrees of freedom to distribute strain, relieve localized stress concentrations, and achieve curvature matching. This geometry-driven behavior is the hallmark of mechanical metamaterials, where global deformation arises from programmed structural motifs rather than bulk material softening. A second key aspect is the auxetic-inspired ligament architecture. Although the disc does not exhibit a bulk negative Poisson’s ratio, the ligament units follow the deformation mechanisms observed in classical auxetic systems such as re-entrant, rotating-square, and rotating-triangle structures33, 34. When the flat disc is pressed onto the curved cornea, each ligament undergoes outward rotation and geometric unfolding, effectively increasing its arc length. This mirrors the kinematics of auxetic mechanisms in which lateral expansion accompanies axial stretching as illustrated in Fig. 2a. The ligament-level behavior, hinge-like rotation at the central waist and widening at the ends (see Fig. S1e, Fig. 2, Video S2 and S3), demonstrate the same rotational-dilatational motion characteristic of auxetic lattices.
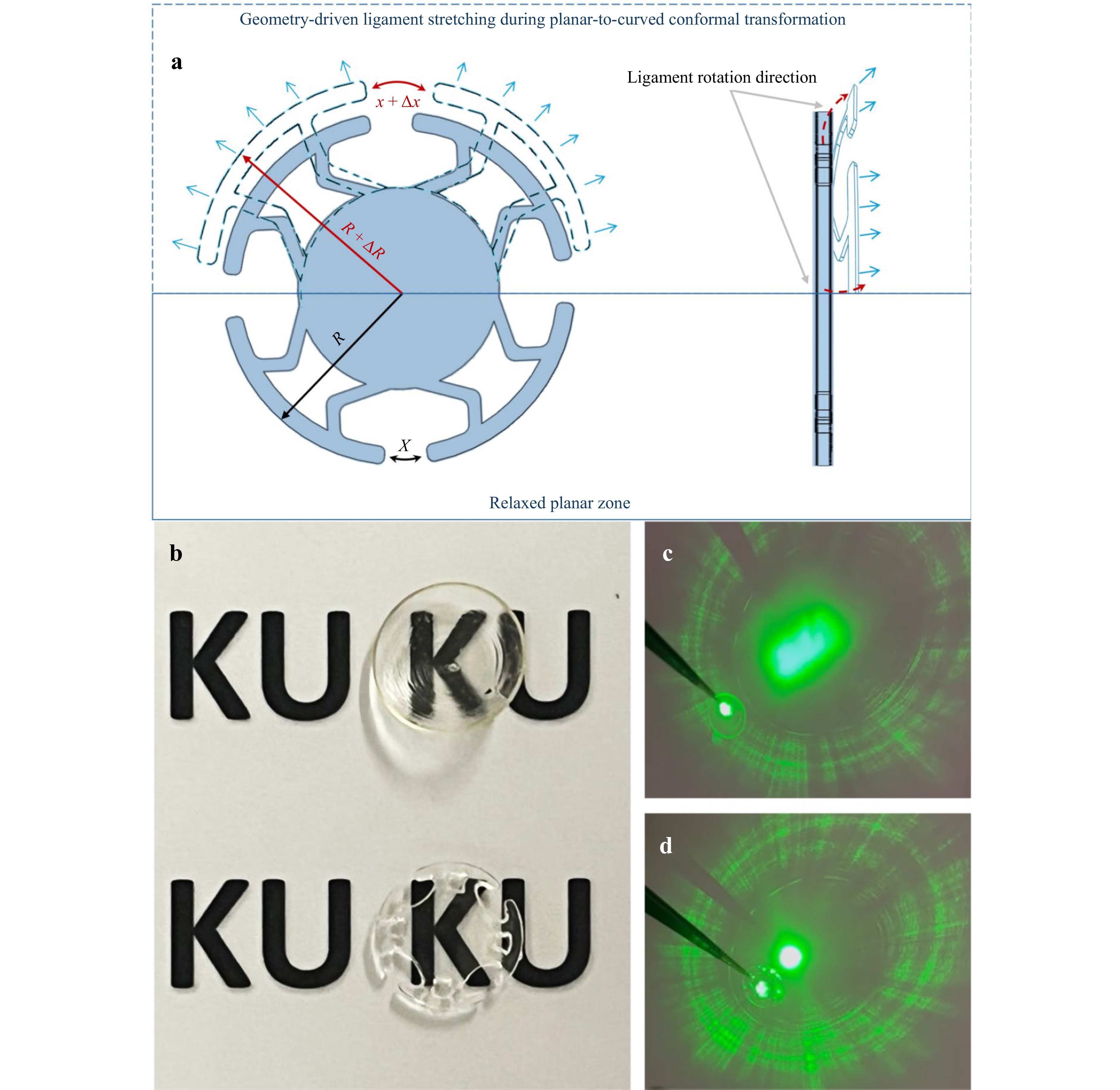
Fig. 2 a This illustration shows that, upon contact with a hemispherical cornea, the flat disc deforms through outward rotation, geometric unfolding, and circumferential arc-length expansion, mimicking the kinematic features characteristic of auxetic-inspired metamaterial behavior. b Optical clarity of the 3D-printed lens. c-d Comparison of laser focusing through a conventional hemispherical 3D-printed lens and the proposed flat ocular disc, demonstrating that staircase-induced surface irregularities in the hemispherical geometry result in focal distortion and increased light scattering, whereas the flat ocular disc enables a more uniform and well-defined focal spot.
Taken together, the circumferential ligament system in this work is intentionally designed according to principles drawn from metamaterials and auxetics. Each ligament functions as a compliant rotational unit capable of controlled outward opening or inward folding, enabling the initially flat disc to morph smoothly onto a hemispherical profile as shown in Video S1. This geometry-programmed deformation, analogous to re-entrant and rotating-unit auxetic architectures33, 34, allows the structure to achieve curvature-adaptive morphing that would be impossible for a monolithic hydrogel disc of similar thickness. Thus, the proposed ocular disc operates as a 2D mechanical metamaterial, wherein distributed flexural hinges and tailored connectivity provide a kinematic pathway for conformal adaptation. Accordingly, the proposed ocular lens can be classified as an auxetic-inspired, metamaterial-based ocular lens design. Further details on the design evolution and the underlying rationale for the auxetic-inspired metamaterial ocular lens are provided in Section S1 (Supplementary Material).
The CAD models of these discs were developed using SolidWorks® 2019 (Dassault Systèmes) and exported in STL format. These files were processed using Chitubox slicing software, with a layer thickness of 35 µm. The discs were fabricated via digital light processing (DLP) technique using a Wanhao Duplicator D8 desktop 3D printer equipped with a 405 nm UV light source. Printing employed an in-house formulated photocurable resin, upon uniform UV exposure, the resin underwent photopolymerization, forming a solid crosslinked hydrogel network. The DLP printing parameters included a bottom exposure time of 120 s of initial 5 layers, followed by a layer exposure time of 80 s per layer, at a printing speed of 30 mm h−1 (refer Table S1, Supplementary Material). All samples were printed parallel to the build plate to ensure consistent surface orientation. A PVC film was adhered to the build plate (see Fig. 1d) to minimize surface artifacts by preventing build roughness from imprinting on the ocular disc27 (see Fig. S2, Supplementary Material). Following 3D printing, the hydrogel specimens were gently wiped with PVC film to remove residual uncured resin from the surface and subsequently UV-cured for 10 minutes in a UV chamber. No additional post-curing treatments were applied. (Refer to Table. S1, Supplementary Material). Additionally, the 3D-printed ocular discs were tinted using Piccaso ink (see Fig. S3, Supplementary Material) by carefully applying the dye onto the surface, followed by air drying under ambient conditions.
-
Surface roughness analysis was performed using a laser profilometer (Olympus OLS5100, Japan) to identify printing-induced artifacts by comparing the surfaces of the 3D-printed ocular disc and reference lenses used in previous study15. Scanning was conducted in auto-acquisition mode with a laser brightness of 55.9 W·cm−2·sr, employing the 3D Standard + Color mode for detailed topographical mapping. To complement the profilometric data, scanning electron microscopy (SEM) was employed for detailed surface morphological analysis. SEM imaging was conducted using a Nova NanoSEM 650 (FEI Co., USA) at an accelerating voltage of 15 kV. Prior to imaging, specimens were sputter-coated with a 12 nm gold (Au) layer to enhance conductivity and resolution, particularly for capturing features on the 3D-printed surfaces.
-
The 3D-printed hydrogel discs were first dried in an oven at 60 °C for 24 h, and the dry weight (Wdry) was recorded. Subsequently, the samples were immersed in phosphate-buffered saline (PBS) solution at ambient temperature (~25 °C) to evaluate swelling behavior over a period of 1440 minutes. At predetermined time intervals, each specimen was carefully removed using tweezers, gently blotted with filter paper to remove surface moisture without applying pressure, and immediately weighed to obtain the swollen weight (Wswollen). The swelling kinetics were assessed by plotting Wswollen over time, and similarly, water absorption characteristics were also calculated using the following equations18:
$${\rm{ Swelling\; kinetics}}\; ({\text{%}}) =\frac{{W}_{\rm swollen}-{W}_{\rm dry}}{{W}_{\rm dry}}\times 100 $$ (1) $$ {\rm{Water\; content}}\; ({\text{%}}) =\frac{{W}_{\rm swollen}-{W}_{\rm dry}}{{W}_{\rm swollen}}\times 100 $$ (2) In hydrogels, oxygen permeability (Dk) is primarily mediated through water, making it directly dependent on the equilibrium water content. This relationship is expressed in Eq. 335:
$$ D_{k} =~1.67{e}^{0.0397~\times w\mathrm{ater}~\mathrm{content}~({\text{%}})} $$ (3) -
To evaluate the crosslinking efficiency (gelation), gel fraction tests were performed on 3D-printed hydrogel discs with a diameter of 1 cm. Freshly printed samples were first dried in an oven at 60 °C for 24 h, and their initial dry weight (W0) was recorded. The dried specimens were then immersed in ethanol and soaked at ambient temperature (~25 °C) for 24 h to extract the soluble, non-crosslinked components. After soaking, the samples were rinsed with fresh ethanol and re-dried under the same conditions as in the initial drying step. The final dry weight (W1) was then measured. The gel fraction (%) was calculated using the following equation:
$$ {\rm{Gel\; fraction}}\; ({\text{%}}) =\frac{{W}_{1}}{{W}_{0}}\times 100 $$ (4) -
The surface contact angle was measured using the sessile drop method36 on both as-printed and PBS-hydrated hydrogel discs, using a custom-built setup equipped with a camera and light source as shown in Fig. S5 (Supplementary Material). A 3 μL droplet of deionized water was deposited on the sample surface, and the contact angle measurements were obtained via ImageJ image analysis software. For optical characterization, the transmittance and absorbance spectra of both transparent and tinted 3D-printed discs were recorded using a UV-vis spectrophotometer (USB 2000+; Ocean Optics) across the 400-800 nm wavelength range (see Fig. S7, Supplementary Material).
-
To assess the thermal stability of the 3D-printed ocular discs, thermogravimetric analysis (TGA) and differential scanning calorimetry (DSC) were performed using a Netzsch STA 449 F5 Jupiter. Measurements were conducted under a nitrogen atmosphere (flow rate: 50 mL·min−1) over a temperature range of 25−600 °C, with a heating rate of 10 °C·min−1. Samples (<10 mg) were placed in alumina crucibles, and thermal transitions, including glass transition temperature (Tg) and thermal degradation behavior, were recorded, considering the relevance of thermal exposure during sterilization processes in ocular applications.
Fourier-transform infrared (FTIR) spectroscopy was also conducted using a Thermo Fisher Nicolet iS50 spectrometer in the range of 4000−500 cm−1 to analyze the chemical structure of the uncured resins constituents and the 3D-printed hydrogels.
-
The rheological behavior of 3D-printed hydrogels is critical for evaluating their durability under ocular conditions, particularly in response to blinking pressure, as well as during lens application and removal. To assess their mechanical resilience and flow behavior, rheological measurements were conducted at ambient conditions using a TA Instruments Discovery Hybrid Rheometer HR30. Key viscoelastic properties, including the storage modulus ($ {G}^{'} $) and loss modulus ($ {G}^{''} $), were evaluated through oscillatory tests under (i) strain-dependent (0.01−100%), and (ii) angular frequency-dependent (0.1−100 rad s−1) conditions. Self-healing behavior was examined through cyclic strain tests by alternating between high (500%) and low (1%) strain over two cycles. In addition, steady shear measurements were performed to investigate shear-thinning behavior, recording viscosity over a shear rate range of 0.01−10 s−1.
-
Mechanical performance was evaluated through quasi-static tensile, compression, flexural, and tear tests conducted on bulk specimens in both as-printed and PBS-hydrated conditions (soaked for 24 h) to simulate ocular environments. Given the continuous exposure of ocular devices to tear fluid, hydration was considered essential for realistic mechanical assessment. All tests were performed using a Zwick-Roell Z005 universal testing machine equipped with a 2.5 kN load cell. Tensile and compression tests were conducted at a crosshead speed of 5 mm·min−1, while flexural tests were performed at 1 mm·min−1, under ambient conditions (25 °C). Dogbone specimens with a gauge section of 37 × 5 × 2 mm3 were prepared for tensile testing, while 12.5 mm dia and 12.5 mm height cylinders and 80 × 12.7 × 3.2 mm3 rectangular bars were fabricated for compression and flexural testing, respectively (as shown in Fig. 8e). Flexural tests were conducted using a three-point bending configuration with a fixed support span of 50 mm. The acquired force vs. displacement data were post-processed to determine elastic moduli (E), tensile/compressive strength ($ {\sigma }_{T/C} $), elongation at break ($ {\varepsilon }_{b} $), flexural strength ($ {\sigma }_{f} $), flexural modulus (Ef), and flexural deflection ($ {\varepsilon }_{f} $) using standard ASTM D638, D695, and D790 procedures. The properties mentioned were calculated using the following equations:
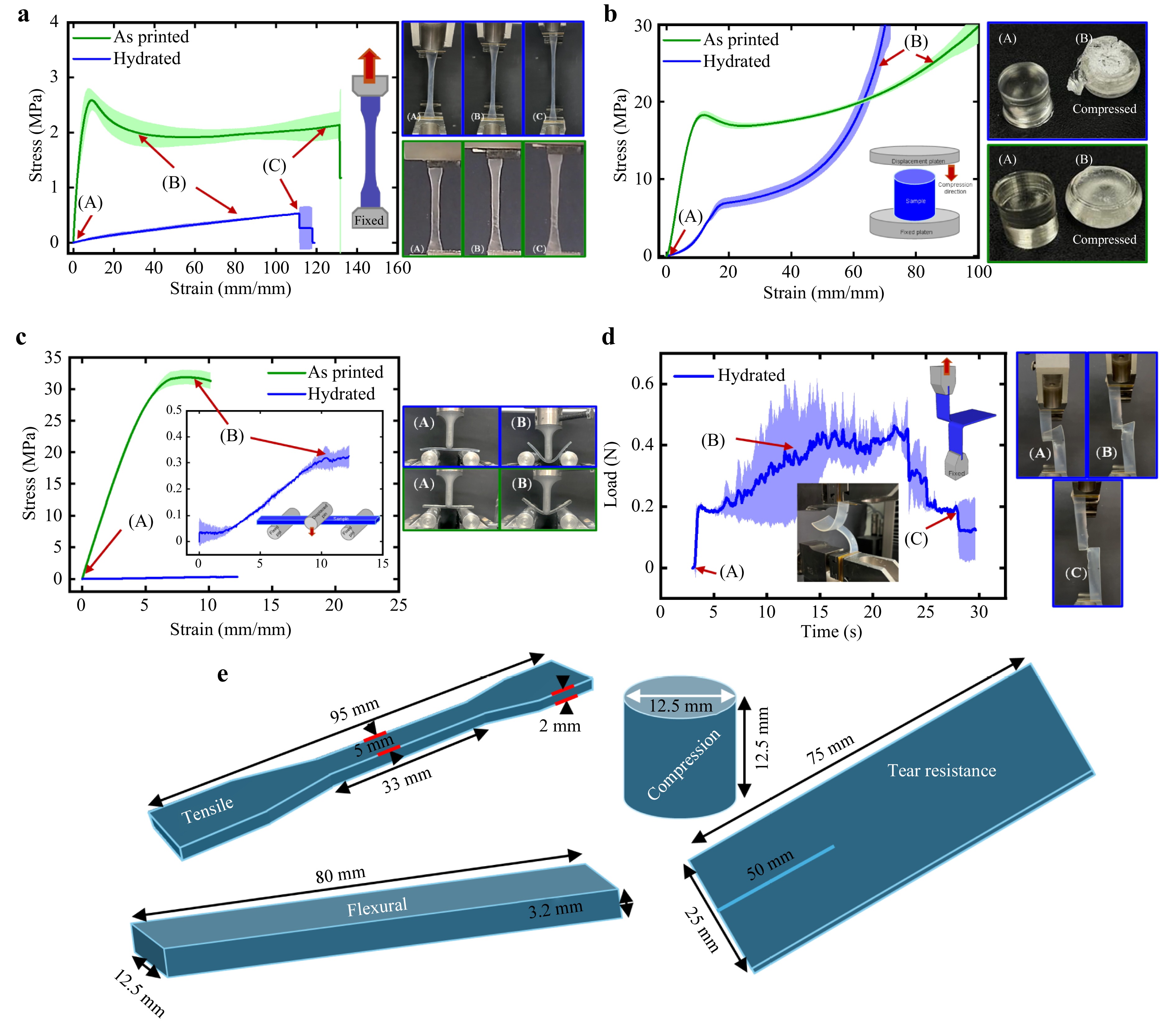
Fig. 8 Mechanical characterization of 3D printed ocular hydrogel material: a tensile testing, b compression testing, c three-point flexural testing, and d tear resistance evaluation. Corresponding deformation images captured during each test provide visual insight into the material’s mechanical response. e Bulk specimens are used for various tests.
$$ {\sigma }_{T/C} = \frac{{F}_{T/C}}{{A}_{cross-section}} $$ (5) $$ {\sigma }_{f} = \frac{3{P}_{i}L}{2b{d}^{2}} $$ (6) $$ {\varepsilon }_{f} = \frac{6Dd}{{L}^{2}} $$ (7) $$ {E}_{f} = \frac{{L}^{3}M}{4b{d}^{3}} $$ (8) where FT/C is maximum force under tension or compression, Across-section is the cross sectional area of the specimen where load is applied, Pi is the applied flexural load at a given point, L is the support span, b is the specimen width, d is the specimen depth, D is the maximum deflection, and M is the slope of the initial linear region of the stress vs. strain curve under bending. The specimen dimensions used for testing are detailed in Fig. 8e. Tear resistance was evaluated using the ASTM D1938 single-tear method, which measures the force required to propagate a tear in thin films (< 2 mm thick). This test was performed to assess the susceptibility of the 3D-printed discs to tearing under blink-induced stress, simulating real-world ocular conditions. PBS hydrated specimens (for 24 h) were prepared as 75 mm × 25 mm strips with a 50 mm central slit introduced using a sharp razor blade (Fig. 8e). Testing was conducted using a constant-rate-of-grip separation setup, with an initial grip separation of 50 mm and a crosshead speed of 250 mm·min−1. Each tongue of the slit was held in an opposing grip, and the tear force was determined from the load vs. time response. For all mechanical tests, results were averaged over 3−5 specimens to ensure reproducibility.
-
The conformal auxetic-inspired metamaterial ocular disc, developed with the aim of functioning as a contact lens, was fabricated using Digital Light Processing (DLP) additive manufacturing. This technique relies on the photopolymerization of resin upon exposure to a specific wavelength of UV light, enabling the formation of a solid hydrogel network. Based on extensive literature evidence, hydrogels derived from HEMA and PEGDA have been widely recognized as suitable candidates for 3D-printed contact lenses due to their optical clarity, biocompatibility, and tunable mechanical properties15, 16, 18, 19.
It is acknowledged that the HEMA - PEGDA hydrogel system itself is not novel. However, the specific composition adopted in this study (97:3 HEMA:PEGDA) was intentionally selected based on reports indicating that hydrogels with a high HEMA content exhibit mechanical and optical properties comparable to those of commercial contact lens materials37, with oxygen permeability often being the main limitation. In contrast, most existing studies employ near-equimolar (1:1) HEMA-PEGDA ratios, which typically yield stiffer, less flexible networks18. Our aim here therefore is to develop an in-house formulation tailored for conformal ocular disc fabrication, prioritizing flexibility, optical clarity, and hydration behavior rather than introducing a new chemistry. The high-HEMA composition is chosen to emulate the property range of commercial lenses, and the performance metrics presented in this study support this rationale.
In this study, a hydrogel formulation based on HEMA and PEGDA was adopted to realize the novel conformal auxetic-inspired metamaterial ocular disc, addressing the limitations reported in prior designs15, 18. The successful fabrication of the ocular disc using DLP is demonstrated in Fig. 1e (also see Figs.S1, S2 and S3, Supplementary Material). These figures illustrate how 3D printing enables precise control over geometry and dimensions, owing to the flexibility offered by computer-aided design (CAD).
Previous studies, including those by Alam et al. and Hisham et al.15, 16, 18, 27, have reported significant surface irregularities in 3D-printed hemispherical contact lenses. These irregularities, primarily due to the staircase effect inherent in layer-by-layer printing, negatively affect wearer comfort. In DLP, the CAD model is first sliced into layers defined by a critical process parameter, layer thickness. Each layer is then sequentially cured by UV exposure over a defined exposure time18. During this process, the previously cured layer is already solidified when the next one is exposed, leading to step-like surface artifacts along curved geometries, especially in hemispherical lenses18, 27. Hence, the previous reports have demonstrated that DLP printing of curved contact lenses (thin, soft, and fragile structures) has proven to be very challenging in terms of print time, intensive post-processing, and support structures required. DLP printing of curved contact lenses is also a labor-intensive process with low repeatability.
To address these aspects, the current design eliminates the need for printing a hemispherical curved surface by introducing a flat disc architecture with auxetic metamaterial ligaments around its circumference (Fig. 1c and 2a). This geometry allows the flat disc to morphologically adapt to the curvature of the human eye, effectively simulating a hemispherical profile without requiring the printing of a curved shell. Consequently, all printed layers remain aligned within a single planar axis, inherently eliminating the staircase effect. Furthermore, a preliminary evaluation of the disc’s conformal-fit behavior under PBS loading including its resistance to lifting and its stability on a spherical eye model and within an artificial anterior chamber (Fig. S6, Supplementary Material) is presented in Section S5 of the Supplementary Material, with corresponding demonstrations provided in Videos S4-S6.
In comparison to traditional hemispherical 3D-printed contact lenses, the proposed ocular disc employs a network of strategically arranged ligaments that function as compliant hinges, allowing the flat disc to fold and stretch upon placement on the eye. These ligaments introduce additional degrees of freedom in bending and in-plane deformation, enabling the structure to conform to the corneal curvature despite being fabricated entirely in a flat configuration an adaptation that is not feasible with a monolithic disc (see Section S1, Supplementary Material).
From both manufacturing and optical perspectives, printing the lens in a flat state eliminates steep overhangs, support structures, and the pronounced inter-layer “staircase” artefacts typically associated with directly printing curved hemispherical lenses. Consequently, the slicing-induced interface marks are minimized, resulting in a substantial improvement in surface smoothness and a reduced likelihood of unintended light scattering or refractive artefacts issues well known for 3D-printed ocular devices. As demonstrated in Fig. 2c-d, laser transmission tests reveal that the traditional hemispherical design produces a dispersed array of focal points due to scattering from the layer-induced ridges, whereas the flat-printed ocular disc produces a single, clean focal point, confirming the optical benefits of the flat, planar fabrication approach.
Furthermore, the flat-printing strategy markedly enhances throughput: the total fabrication time is reduced from approximately 5 h 40 min to ~40 min (≈88% reduction), which is advantageous for rapid prototyping as well as potential manufacturing scale-up. Collectively, these improvements enhanced conformability via ligament-mediated flexibility, superior surface quality with reduced scattering risk, and significantly shorter production times underscore the advantages of the proposed architecture. Beyond these benefits demonstrated, additional performance enhancements are anticipated, and several ongoing studies are already yielding encouraging preliminary results that will be disseminated in subsequent, dedicated investigations (Future work). A simple linear elastic simulation was conducted in ABAQUS to compare a conventional contact lens with the proposed conformal, auxetic-inspired metamaterial ocular disc. Eyelid-induced pressure was applied to approximate the dynamic nature of eye blinking. This preliminary analysis provides a qualitative comparison of the two designs and does not fully replicate the complex physiological conditions of the ocular environment; further details are provided in Section S7 of the Supplementary Material.
-
To validate the surface quality, laser profilometry was performed on both the novel ocular disc and a 3D-printed hemispherical contact lens. As shown in Fig. 3a (top), the conformal auxetic-inspired metamaterial ocular disc exhibits a smooth and uniform surface with minimal variation in height, suggesting low surface roughness. The corresponding 2D height map reveals predominantly green regions, indicating that the surface lies within a narrow height range on the color scale (–23.35 µm to +22.37 µm), with no significant surface artifacts. In contrast, Fig. 3a (bottom) depicts the surface of the 3D-printed hemispherical lens, which shows distinct periodic ridges and valleys. These features are characteristic of layer-by-layer printing artifacts, as confirmed by the 2D height map, where intense color variations (blue to red) reflect significant topographical fluctuations up to approximately ± 550 µm. This non-uniformity is attributed to the cumulative layer-wise build process. Further confirmation is provided by SEM micrographs (see Fig. 3b), which reveal the smooth surface morphology of the conformal auxetic-inspired metamaterial ocular disc, while clearly capturing the layer lines and printing marks on the hemispherical contact lens.
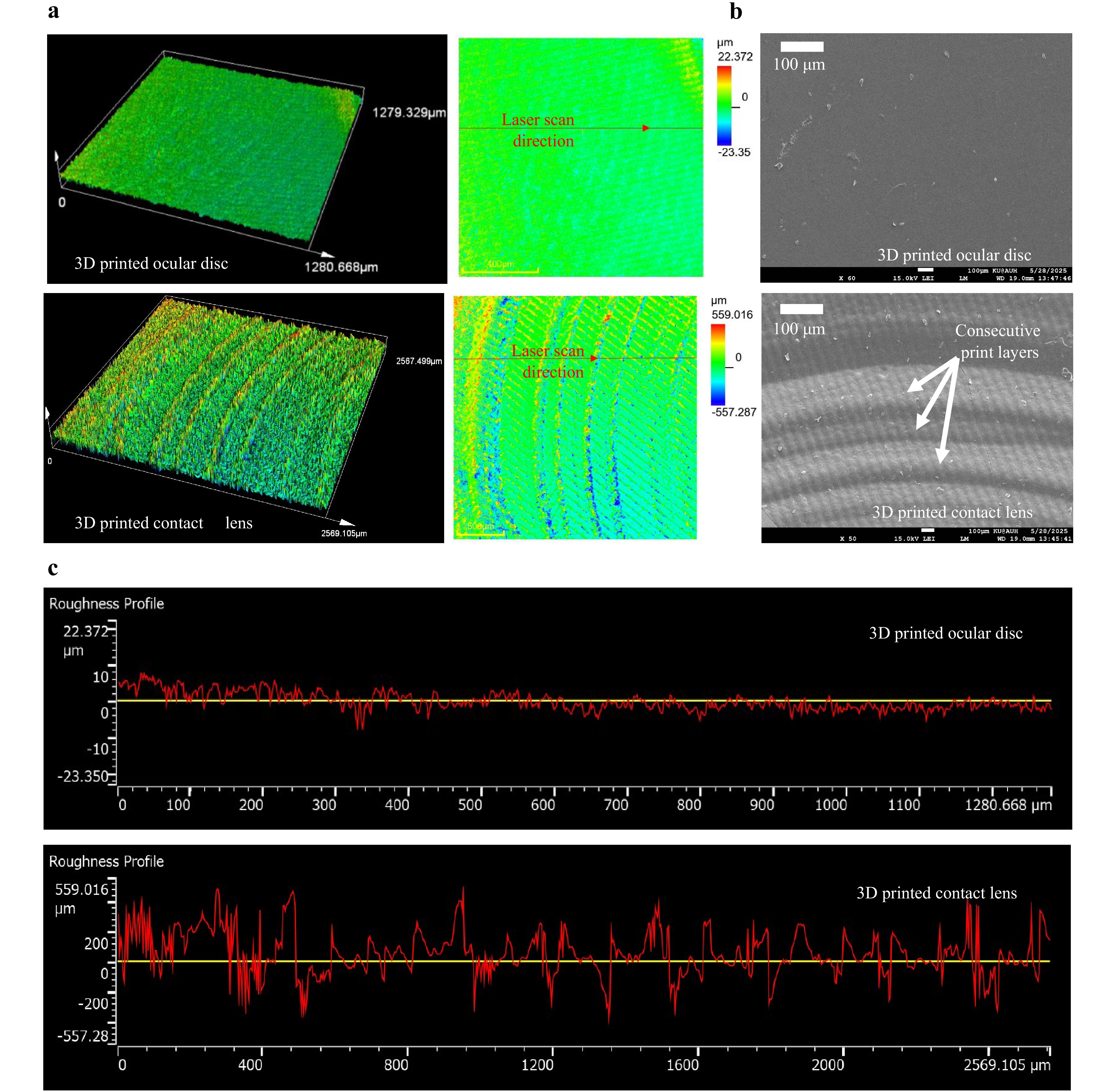
Fig. 3 Surface characterization of the 3D printed conformal auxetic-inspired metamaterial ocular discs: a surface topography captured using a laser profilometer, b SEM micrographs showing surface morphology of the 3D printed ocular discs and 3D printed hemispherical contact lenses. c Quantitative surface roughness profiles obtained from laser profilometry analysis.
Quantitative surface roughness analysis (see Fig. 3c) reinforces these observations. The root mean square roughness (Rq) of the conformal auxetic-inspired metamaterial ocular disc was measured to be 1.781 µm, significantly lower than that of the hemispherical (curved) lens, which exhibited an Rq value of 139.602 µm both 3D printed. This nearly 98% reduction in surface roughness highlights the efficacy of the flat ocular lens design in achieving a surface smoothness approaching optical-grade quality, without the need for complex post-processing (surface area scans are attached in Fig. S4, Supplementary Material). Future studies will focus on enhancing surface quality by employing higher-resolution 3D printing systems and integrating post-processing methods such as controlled polishing, surface smoothing, and tailored photopolymer-curing strategies which are known to further reduce roughness toward optical-grade standards.
-
To investigate the hydration characteristics of the 3D printed hydrogel-based ocular discs, water absorption and swelling kinetics were assessed by immersing the dried samples in phosphate-buffered saline (PBS) at room temperature. Measurements were recorded at regular time intervals until equilibrium was reached, using at least 3−5 samples. Consistent data sets were averaged for analysis (see Fig. S10, Supplementary Material). Fig. 3 presents the hydration behavior of the hydrogel over a 1440-minute period.
Both the water content and swelling kinetics exhibited a typical biphasic swelling profile, characterized by a rapid initial uptake of water, followed by a plateau phase, indicating the attainment of swelling equilibrium. Notably, the novel ocular disc achieved approximately 95% of its maximum water absorption (see Fig. 4a) and swelling (see Fig. 4b) within the first 120 minutes, demonstrating decent hydration behavior.
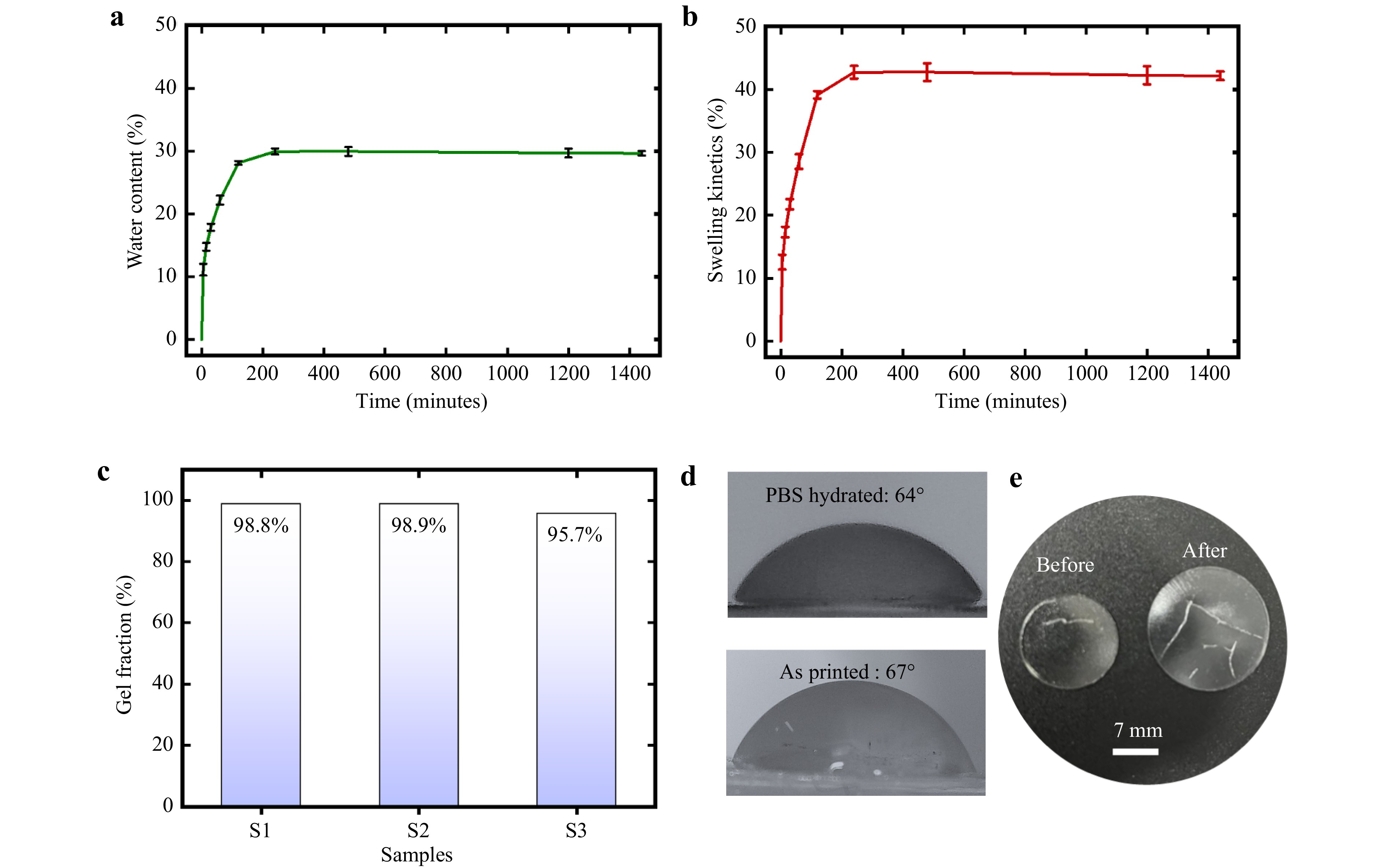
Fig. 4 Physicochemical characterization of the 3D printed ocular hydrogel discs: a water absorption behavior over time, b swelling kinetics in PBS solution, c gel fraction indicating crosslinking efficiency, and representative images captured during d contact angle measurements to assess surface wettability and e visuals of the sample before and after the gel fraction test.
This fast swelling can be attributed to the hydrophilic nature of the HEMA-PEGDA hydrogel network, which facilitates rapid water diffusion into the polymer matrix. The inclusion of PEGDA, a flexible and highly hydrophilic crosslinker, plays a critical role in enhancing the network’s free volume, thereby promoting faster curing kinetics and enhances print fidelity.
The equilibrium water content (~30%) of the conformal auxetic-inspired metamaterial ocular disc demonstrates its hydration capacity, achieved within 4 hours, a crucial factor for ocular comfort, oxygen permeability, and biocompatibility in contact lens applications. Commercially available hydrogel lenses typically exhibit water absorption in the range of 30% to 80%7, 35, positioning the current design within the optimal range. Further enhancement in water content may be achievable through the incorporation of suitable additives. Moreover, the rapid swelling kinetics indicate favorable mechanical softness and flexibility, enabling the lens to quickly hydrate upon insertion, which is a highly advantageous feature for in situ ocular deployment.
The plateauing (equilibrium) behavior observed at ~42% swelling further suggests excellent structural stability, with no evidence of degradation or delayed secondary swelling phases throughout the measurement period. This highlights the uniformity and reproducibility of the photopolymerization process employed in DLP-based fabrication.
Importantly, the novel design incorporates strategically placed open-cell geometries that may enhance oxygen diffusion to the corneal surface, one of the primary design objectives for long-wear ocular devices. Oxygen permeability (Dk) was estimated based on water content using ISO 18369-4 guidelines (equ. 3), where the measured ~30% water content corresponded to a Dk value of approximately 5.49. Although this value is lower than those reported for commercial silicone hydrogel lenses, it is comparable to that of several commercial hydrogel-based lenses38, confirming the suitability of the material for short-to-medium duration use. Future work will focus on integrating silicone-based monomers into our photocurable resin to enhance Dk while retaining the benefits of our flat-printing design.
To assess the degree of crosslinking, gel fraction analysis was conducted. The average gel fraction of 97.8%, as shown in Fig. 4c, indicates a highly crosslinked network with minimal leaching, supporting material integrity during sterilization and extended wear. This also indicates that the print parameters and monomer/crosslinker ratios are well optimized, achieving adequate polymerization within the printed layers.
Surface wettability was evaluated through contact angle measurements performed on both as-printed and PBS-hydrated conformal auxetic-inspired metamaterial ocular discs. As shown in Fig. 4d, the contact angles were 67° (average 67.1° ± 0.85) in the as-printed state and decreased to 64° (average 64.62° ± 0.56) upon hydration (Trail values are provided in Table S2, Supplementary Material). Given that contact lenses are typically used in a hydrated condition, the latter value is more representative of their practical performance. These values fall within the typical range reported for commercial contact lenses (44−79°)12, 39, 40. Since a contact angle below 90° indicates hydrophilic behavior41, and lower values are associated with increased surface wettability, the results confirm the sufficient hydrophilicity of the fabricated ocular disc for real-life ophthalmic applications.
Taken together, these results confirm that the 3D printed conformal auxetic-inspired metamaterial ocular disc exhibits optimal hydration dynamics, structural stability, oxygen permeability, and surface wettability, making it a promising candidate for next generation contact lens materials, particularly in applications demanding rapid hydration and sustained water retention.
-
The optical transmission spectra of 3D printed hydrogel-based discs are presented in Fig. 5. The transparent, untinted disc in its as-printed state exhibited high optical transparency, with an average transmission of approximately 95% across the visible spectrum (400−800 nm). This high transmittance is attributed to the uniform polymer network and the absence of light-scattering inhomogeneities, which confirms the optical clarity of the printed disc in its dry state. High optical transmission (low scattering losses) also alludes to the uniform printing of layers and smooth interlayer interfaces formed, without defects and air bubbles.
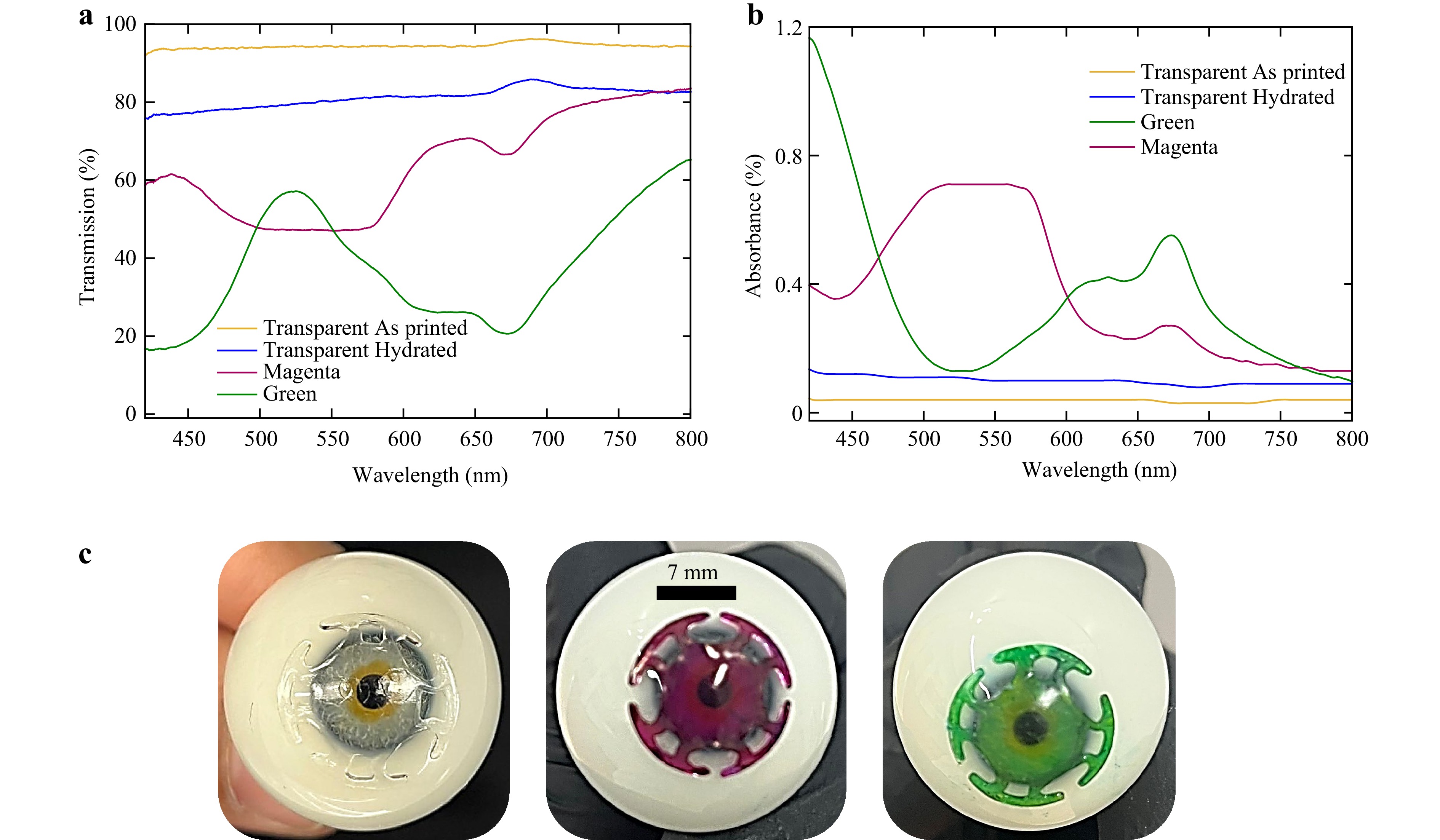
Fig. 5 Optical characterization of 3D printed auxetic ocular discs: a transmittance and b absorbance spectra as a function of wavelength for both transparent and tinted samples, highlighting the effect of tinting on light modulation properties. c Transparent and tinted 3D printed ocular disc using piccassio ink inserted on an eye model.
Upon hydration in phosphate-buffered saline (PBS), the average optical transmittance slightly decreased to ~83%. This reduction is likely due to increased light scattering caused by water uptake and the subsequent microstructural swelling of the hydrogel matrix. Such behavior is consistent with previously reported hydrogel systems42. Nonetheless, the hydrated ocular discs still demonstrate acceptable optical performance for ocular applications.
In contrast, tinted discs exhibit distinct wavelength-dependent transmission dips, enabling selective light filtering. 3D printed ocular disc embedded with magenta dye displayed a pronounced absorption band centered at ~530 nm, with a full width at half maximum (FWHM) ranging from 425 to 575 nm, effectively blocking green wavelengths. Meanwhile, green-tinted discs demonstrated two significant absorption regions, one centered around 400 nm, filtering UV and violet light, and another centered around 675 nm (FWHM: 550−750 nm), filtering far-red light. These tailored spectral responses indicate the potential for engineering application-specific optical properties, such as UV and blue light filter or contrast enhancement in visual aids.
Collectively, these findings underscore the versatility of DLP-based 3D printing for fabricating optically tunable hydrogel lenses. Through careful dye incorporation and formulation optimization, custom spectral transmission profiles can be achieved to suit various ophthalmic applications.
-
The thermal stability and phase transitions of the 3D printed hydrogel were investigated using thermogravimetric analysis (TGA) and differential scanning calorimetry (DSC). The TGA curve (red) reveals the hydrogel’s weight loss profile under controlled heating (see Fig. 6a). An initial minor weight loss occurs below 100 °C, which is attributed to the evaporation of physically adsorbed moisture. This is followed by a major weight loss between approximately 300 °C and 450 °C, corresponding to the thermal decomposition of the polymeric network. Beyond 500 °C, the remaining mass plateaus, indicating the formation of a thermally stable char residue.
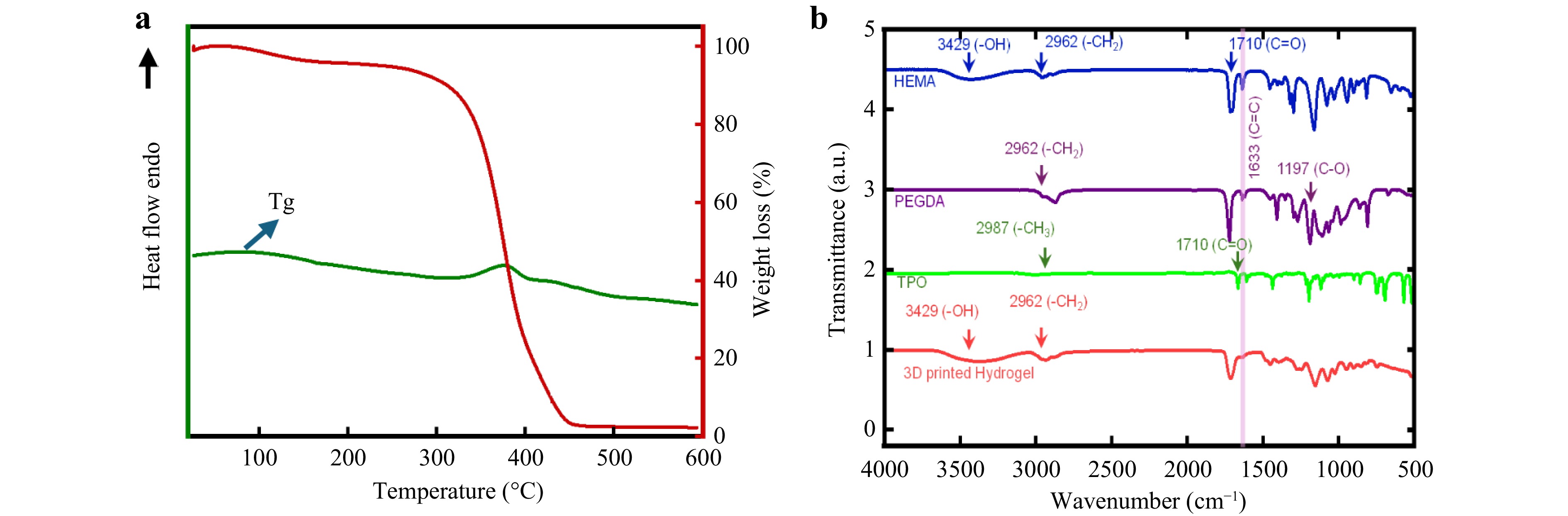
Fig. 6 Thermal and chemical characterization of 3D printed hydrogel discs: a DSC and TGA curves illustrating thermal transitions and stability. b FTIR spectra showing characteristic functional groups and chemical composition.
Complementary insights are provided by the DSC thermogram (green) in Fig. 6a, which reflects the heat flow associated with physical and chemical transitions in the hydrogel. A subtle endothermic peak below 100 °C is consistent with the loss of bound water. Notably, the absence of a clear melting transition suggests that the hydrogel is either amorphous in nature or possesses a highly crosslinked network, which suppresses crystallinity and inhibits melting behavior. An inflection in the DSC heat flow between 300 °C and 400 °C aligns closely with the primary degradation phase observed in the TGA curve. This transition likely represents an exothermic decomposition of the hydrogel matrix, consistent with the breakdown of the polymer backbone.
Together, the TGA and DSC results confirm that the hydrogel exhibits thermal stability up to approximately 300 °C, beyond which thermal degradation dominates. These findings are particularly critical for guiding the design of sterilization protocols for the 3D printed ocular hydrogel lenses. The material’s ability to retain structural integrity at elevated temperatures ensures compatibility with thermal sterilization methods, while also confirming its robustness under physiological and processing conditions.
FTIR analysis was performed in the range of 500-4000 cm−1 with 32 scans per spectrum to confirm the chemical composition and successful photopolymerization of the 3D printed hydrogel based on HEMA, PEGDA, and TPO. As shown in Fig. 6b, the individual spectra of the precursors exhibit their characteristic peaks: HEMA shows -OH stretching at 3429 cm−1 and C = O stretching at 1710 cm−1; PEGDA displays -CH2 stretching at 2962 cm−1, C = O at 1710 cm−1, and C-O at 1197 cm−1; and TPO presents a -CH3 peak at 2987 cm−1. The final 3D-printed hydrogel spectrum retains key absorption bands at 3429 cm−1 (-OH), 2962 cm−1 (-CH2), and a shifted C = O peak at 1633 cm−1, confirming network formation. The disappearance of residual monomer peaks indicates complete polymerization and effective crosslinking, validating the chemical integrity of the hydrogel for ocular applications.
-
The rheological performance of conformal auxetic-inspired metamaterial hydrogel-based ocular discs is a critical factor influencing their functionality under physiological conditions such as eye movement, blink-induced pressure, lens insertion, and removal. In this study, the rheological behavior of 3D printed hydrogel discs, pre-hydrated in phosphate-buffered saline (PBS) for 24 hours, was systematically evaluated, focusing on their shear-thinning and self-healing capabilities. For statistical consistency, this test was performed on 3 replicates (see Fig. S11, Supplementary Material), and one representative curve is presented as shown in Fig. 7a-d.
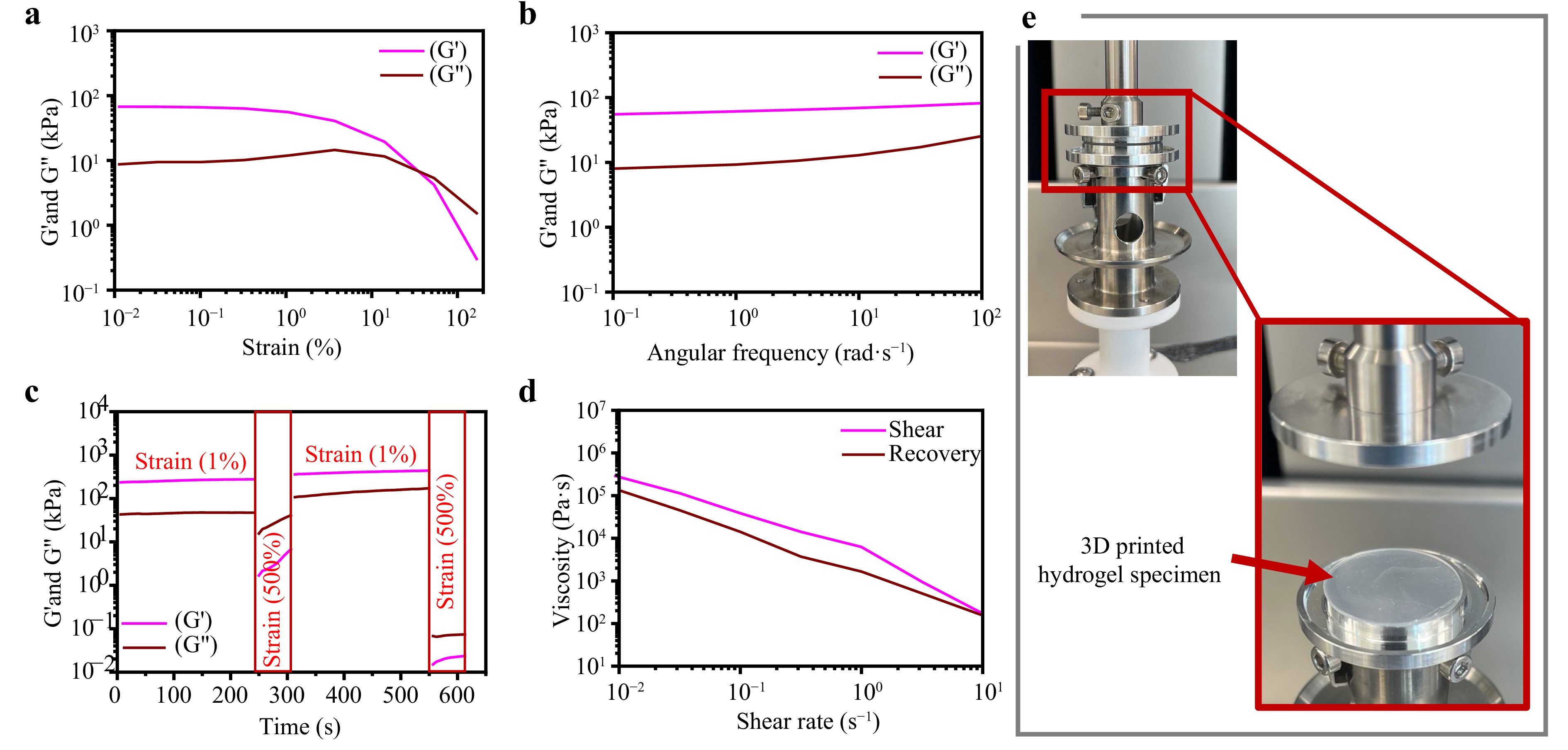
Fig. 7 Rheological analysis of the 3D printed hydrogel discs hydrated in PBS: a strain-dependent oscillatory shear response, b frequency-dependent oscillatory shear behavior, c assessment of self-healing capability through step-strain tests alternating between 1% and 500% strain, and d demonstration of shear-thinning behavior and structural recovery under varying shear rates. e Experimental setup and the printed samples used for the rheological analysis.
Oscillatory strain-sweep tests revealed the viscoelastic nature of the hydrogels, with the storage modulus ($ {G}^{'} $) exceeding the loss modulus ($ {G}^{''} $) within the linear viscoelastic regime. A pronounced shear-thinning response was observed, with the hydrogel network maintaining structural integrity up to a strain amplitude of ~40%, at a constant angular frequency (ω = 10 rad/s), as shown in Fig. 7a. Further, frequency-sweep measurements at a constant strain of 1% confirmed that $ {G}^{'} $ remained consistently higher than $ {G}^{''} $ across the tested frequency range, indicating a predominantly elastic behavior (Fig. 7b). To investigate the self-healing potential, strain-amplitude step tests were performed by alternating the applied strain between 1% and 500% at a constant frequency of 1 rad/s (Fig. 7c). At high strain (500%), both $ {G}^{'} $ and $ {G}^{''} $ significantly decreased, suggesting disruption of the polymer network. Upon reapplication of low strain (1%), the moduli recovered rapidly, demonstrating the reversible restoration of the hydrogel structure. This behavior confirms excellent self-healing performance and resilience of the hydrogel under cyclic deformation.
In addition, a hysteresis loop analysis was conducted by ramping the strain from 0.01% to 10% and subsequently reversing the direction (Fig. 7d). The hydrogel exhibited a reversible viscosity profile, returning to its initial rheological state upon unloading. This dynamic recovery underscores the tunable and resilient rheological properties of the printed hydrogel, which are essential for sustained performance in ocular environments. Collectively, the observed shear-thinning and self-healing behaviors make these materials strong candidates for 3D printed wearable and ophthalmic applications.
-
The mechanical integrity of ocular devices is paramount to ensure reliable handling during application, sustained durability during wear, and overall user comfort. In this study, the mechanical performance of 3D-printed hydrogel used for ocular discs was systematically evaluated under various loading conditions, including tensile, compressive, flexural, and tear resistance, both in the as-printed and post-hydration states in PBS solution. These tests aimed to simulate the mechanical demands the lens may encounter during storage, handling, and real-time ocular usage. All mechanical tests were conducted at ambient room temperature (25 ± 2 °C), using standard testing protocols. For statistical consistency, each test was performed on 3 to 5 replicates (see Fig. S12, Supplementary Material), and the results are presented as average response curves (solid lines) with deviations represented by shaded regions, as shown in Fig. 8a-d. The complete sequence of deformation under each loading scenario is illustrated through the accompanying image frames alongside the corresponding stress vs. strain curves for all tests. The labels marked (e.g. A, B, etc.) on each frame denote the specific points on the curve at which those deformation stages were observed.
Uniaxial tensile testing was performed on dogbone-shaped specimens prepared in accordance with the ASTM D638 standard, suitable for soft polymer materials. The representative stress vs. strain curves for both as printed and hydrated specimens are illustrated in Fig. 8a. Key performance indicators extracted from the curves include the elastic modulus (E), ultimate tensile strength ($ {\sigma }_{S} $), and elongation at break ($ {\varepsilon }_{f} $). The as-printed hydrogel exhibited a tensile strength of 2.57 ± 0.21 MPa, an elastic modulus of 49.6 ± 5.1 MPa, and an elongation at break of 134 ± 3.53%. Upon hydration, these values decreased to 0.52 ± 0.02 MPa, 0.71 ± 0.2 MPa, and 115.2 ± 5.23%, respectively, with modulus matching the commercial contact lens range of 0.2 – 2 MPa7. The reduction in tensile modulus and strength upon hydration indicates a softening effect due to water uptake.
Cylindrical samples were tested under uniaxial compression in accordance with ASTM D695. The stress vs. strain response, presented in Fig. 8b, was used to determine compressive modulus and strength. The as-printed specimens exhibited a compressive strength of 17.74 ± 0.25 MPa and a modulus of 231.93 ± 3.69 MPa, which decreased to 7.12 ± 0.17 MPa and 38 ± 1.41 MPa, respectively, in the hydrated state. This decline in compressive stiffness confirms the hydrogel’s water-responsive mechanical behavior and its implications for load-bearing stability in moist physiological environments such as the eye.
Flexural properties were assessed using a three-point bending configuration as per ASTM D790. The stress vs. strain response shown in Fig. 8c, revealed a similar trend to the tensile and compression tests. The as-printed hydrogel demonstrated a flexural strength of 38.9 ± 1.4 MPa, a flexural modulus of 3202 ± 65 MPa, and a deflection of 7.05 ± 0.06% which reduced to 0.376 ± 0.09 MPa, 17.7 ± 1.73 MPa and 8.64 ± 0.01% after hydration. The observed reduction in flexural rigidity suggests enhanced flexibility and conformability of the hydrated ocular disc, beneficial for in-eye comfort and adaptability to corneal curvature.
To evaluate the lens’s resistance to tearing, an essential property during manual handling and lens durability, a tear test was performed on hydrated specimens following ASTM D1938. The tear strength was determined to be 0.1965 ± 0.017N and a mean tear force of 0.3253 ± 0.1872N from the load vs. time curve (Fig. 8d). This value confirms sufficient mechanical robustness for handling during application and removal.
Across all testing modes (refer Table 1), a consistent trend was observed: the mechanical performance of hydrated samples was lower than that of the as-printed samples. This behavior aligns with the fundamental swelling characteristics of hydrogels, wherein hydration leads to network expansion and increased chain mobility. These outcomes are particularly critical for ocular applications where the lens must balance mechanical robustness during handling with softness and compliance during wear.
As printed PBS hydrated Tensile Elastic Modulus (MPa) 49.6 ± 51 0.71 ± 0.2 Tensile Strength (MPa) 2.57 ± 0.21 0.52 ± 0.02 Elongation at break (%) 134 ± 3.53 115.2 ± 5.23 Compression Elastic Modulus (MPa) 231.93 ± 3.69 38 ± 1.41 Compressive Strength (MPa) 17.74 ± 0.25 7.12 ± 0.17 Flexural Flexural Modulus (MPa) 3202 ± 65 17.7 ± 1.73 Flexural Strength (MPa) 38.9 ± 1.4 0.376 ± 0.09 Deflection (%) 7.05 ± 0.06 8.64 ± 0.01 Table 1. Summary of mechanical properties of 3D printed hydrogel ocular discs in as-printed and hydrated states under different loading conditions.
-
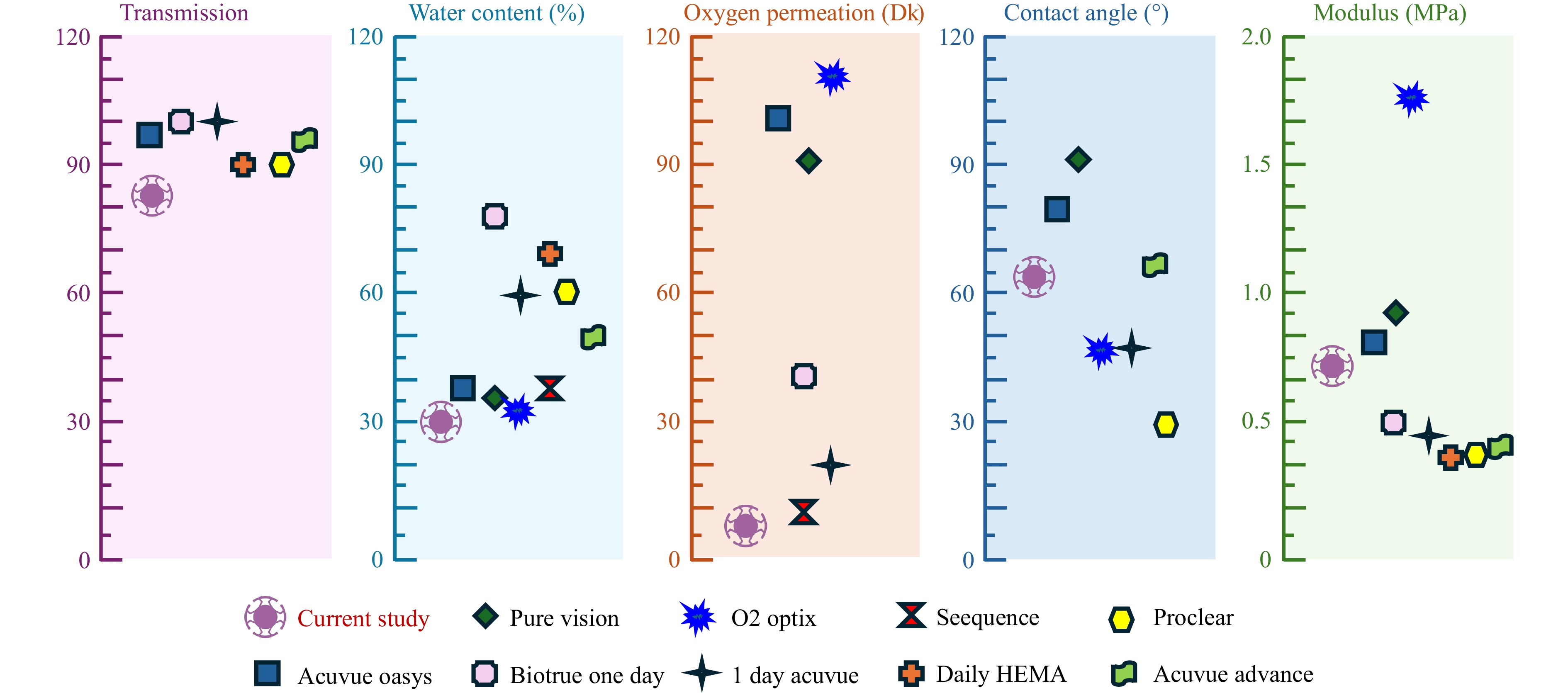
The performance of the 3D-printed conformal auxetic-inspired metamaterial hydrogel-based ocular disc developed in this study is benchmarked against commercially available contact lenses, as shown in Fig. 9. Overall, the proposed design exhibits key performance indicators that fall within the typical range of commercial hydrogel lenses. While the optical transmittance of the 3D-printed disc is slightly lower, it remains within an acceptable range for ocular applications. However, the oxygen permeability is notably lower than that of commercial silicone hydrogel lenses, which benefit from enhanced oxygen transfer through silicone domains. Compared to standard hydrogel lenses such as polymacon (e.g., Seequence), the current design demonstrates comparable permeability. Future work may focus on enhancing oxygen permeability by increasing water content or incorporating silicone into the hydrogel matrix to develop 3D-printed silicone hydrogel discs.
-
This study demonstrates a fundamental shift in the manufacturing paradigm for 3D-printed ophthalmic devices. By replacing the conventional, difficult-to-print curved geometry with a functionally equivalent, flat-printable design, we have overcome the critical barrier of surface roughness inherent to layer-by-layer fabrication. Our conformal, metamaterial-inspired ocular disc achieves near optical-grade surface quality directly from the printer, eliminating the need for additional post-processing apart from UV curing. The design was successfully fabricated using digital light processing (DLP) by polymerizing an in-house formulated photocurable resin. Comprehensive physicochemical, optical, rheological, and mechanical characterizations were performed on both as-printed and PBS-hydrated samples, confirming their suitability for ocular applications. Key findings of this work include the achievement of exceptionally smooth surface morphology, essential for ocular comfort, and a high gel fraction of approximately 97.5%, indicating excellent crosslinking efficiency and material stability. The hydrogel discs demonstrated desirable swelling kinetics and optical clarity, with light transmittance exceeding 83% for untinted ocular discs. Additionally, the incorporation of tinting resulted in distinct spectral modulation, suggesting potential applications for cosmetic enhancements, management of color vision deficiencies, or corrective solutions for color blindness. The thermal analysis confirmed the hydrogel’s thermal stability up to 300 °C, supporting its compatibility with sterilization processes. Rheological evaluation revealed a viscoelastic nature with pronounced shear-thinning behavior, along with excellent self-healing performance, confirming the structural resilience of the hydrogel network. Mechanical testing of PBS-hydrated samples yielded a tensile modulus of ~0.71 MPa, flexural strength of ~0.376 MPa, and tear strength of ~0.2 N, indicating sufficient durability and handling performance for contact lens use. Overall, this study demonstrates the feasibility of a multifunctional ocular disc platform and opens avenues for future developments, including the integration of responsive ligaments for applications such as drug delivery, ocular environment monitoring, and biosensing in next-generation smart contact lenses.
-
The authors acknowledge the use of Zwickiline materials testing machine UTM Model: Z2.5, Netzsch STA 449 F5 Jupiter instrument, Hybrid Rheometer HR30 (TA Instruments), laser scanning profilometer (Olympus OLS5100, Japan) at Khalifa University of Science and Technology (KU-EQP-[Material testing lab and RiC2D]). This research was funded by Khalifa University of Science and Technology through the Research Innovation Grant (RIG), Project ID KU-INT-RIG-2024-8474000736 and the Advanced Digital & Additive Manufacturing (ADAM) Research Group (Award No. 8474000163).
Conformal metamaterial inspired contact lenses−designing, 3d printing and characterization for ocular applications
- Light: Advanced Manufacturing , Article number: 39 (2026)
- Received: 03 October 2025
- Revised: 17 March 2026
- Accepted: 17 March 2026 Published online: 21 April 2026
doi: https://doi.org/10.37188/lam.2026.039
Abstract: 3D printed contact lenses have emerged as promising candidates for advanced ocular applications due to their customizable design and functional versatility. In this study, a novel conformal auxetic-inspired metamaterial ocular disc architecture was developed using digital light processing (DLP), a high-resolution vat photopolymerization technique, and fabricated using an in-house hydrogel formulation. The printed disc was systematically evaluated for its mechanical, optical, and physicochemical performance. Mechanical testing confirmed excellent elasticity and durability, with the hydrated hydrogel exhibiting a tensile modulus of ~0.71 MPa, matching the range of commercial soft contact lenses. Laser profilometry revealed a smooth surface topology essential for user comfort, achieving a root mean square roughness (Rq) of 1.78 µm, a nearly 98% reduction compared to conventionally printed hemispherical lenses. Contact angle measurements (64° hydrated) indicated favorable wettability. Optical characterization exhibited high light transmittance, averaging ~83% across the visible spectrum in the hydrated state. Hydration related properties, including swelling kinetics, water content, and gel fraction, confirmed effective water uptake and retention, supporting oxygen permeability. FTIR spectroscopy validated the chemical integrity of the polymer network, while DSC/TGA analysis confirmed thermal stability up to 300 °C. Furthermore, rheological evaluation indicated a stable viscoelastic profile with notable self-healing behavior. Collectively, this study establishes a 3D printed hydrogel-based conformal metamaterial contact lens platform, offering a promising pathway for the development of next-generation smart ocular devices via additive manufacturing.
Research Summary
Flat-to-Fit 3D Printed Conformal contact lenses: Ocular Applications
Researchers at Khalifa University have developed a novel 3D printed conformal hydrogel ocular lens inspired by auxetic metamaterial design for next-generation contact lens applications. Fabricated using digital light processing and an in-house photocurable hydrogel resin, the flat-printed lens addresses the surface roughness challenges typically associated with curved 3D printed lenses. By enabling planar fabrication, the design significantly reduces build time while eliminating the need for complex support structures or post-processing treatments. The device demonstrated excellent optical transparency, favorable wettability, rapid hydration behavior, and mechanical softness comparable to commercial soft contact lenses. Its smooth surface, structural durability, and stable viscoelastic response highlight its potential for comfortable ocular wear. This work opens new opportunities for personalized, multifunctional, and smart ophthalmic devices enabled by additive manufacturing.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article′s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article′s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.







 DownLoad:
DownLoad: